Poverty and Health Insurance Coverage Among Rural Children
August 2019
by Shawnda Schroeder, PhD
Funded by the Federal Office of Rural Health Policy (FORHP), under the Health Resources and Services Administration (HRSA), the Rural Health Research Gateway strives to disseminate the work of the FORHP-funded Rural Health Research Centers (RHRCs) to diverse audiences. The RHRCs are committed to providing timely, quality research on the most pressing rural health issues. This resource provides a summary of recent research.
Health insurance coverage can influence whether individuals seek care. Studies indicate this is especially concerning for pediatric populations, because dropping in and out of coverage is associated with adverse health outcomes.1 State and federal programs have worked to increase the number of children insured, but there are other factors that can affect health insurance status beyond coverage availability. Specifically for rural children, barriers may include limited resources, poverty, and/or lack of insurance options.1,3-6
Poverty
From 2000-2010, rural counties experienced a 4% decrease in the proportion of the population under the age of 18 (children). Remote rural counties experienced a more significant decrease (9%) than did micropolitan counties (2%).2 Despite this decline in the proportion of the rural population ages 19 or younger, 95 of the 100 counties in 2012 with the highest childhood poverty rates were rural counties.3 The percentage of rural children in poverty or considered low income has increased in both small rural and large rural areas from 2003-2012.4 Hispanic children had the largest increase in the percentage of children living in low-income/poor households between 2003 and 2012; that rate increased from 17.4% to 23.5%.3
Insurance Coverage
In 2011 and 2012, the rate of children (ages 0-17) with health insurance coverage increased to 95% of all children in the U.S. However, health insurance coverage for Hispanic children still lagged behind other race/ ethnicity groups.4 The increase included all types of insurance coverage. Increased Medicaid coverage may have been the result of the Affordable Care Act, Medicaid expansion, and/or the result of parents exploring new healthcare options and learning their children had always been eligible.5
Medicaid is a program for children up to the age of 19 who are at or below a certain percentage of the Federal Poverty Level (FPL). The program is meant to cover low income and poor children. The FPL rate of eligibility is based on individual state guidelines. Regardless of geography, children represent the largest proportion of Medicaid beneficiaries.1 See Figure 1.
Figure 1. Groups Covered by Medicaid, 20121
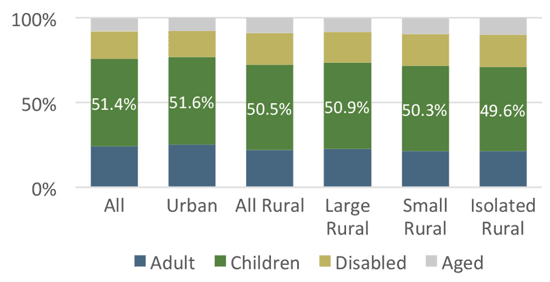
Although data between 2003 and 2012 indicate an increase in the proportion of rural children who were Hispanic and non-White, minority groups still represent a smaller proportion of the overall population in rural communities.4 However Hispanics, American Indians/ Alaska Natives, and Asian/Pacific Islanders present the sharpest increases in the proportion of children covered by Medicaid between urban and more rural communities. See Figure 2. Although only 47.4% of White children in isolated rural communities were Medicaid enrollees, 73.6% of Hispanic children in isolated rural communities were enrolled.1 This correlates with the previously addressed increase in the proportion of Hispanic children living in poverty.3
Figure 2. Distribution of Medicaid Enrollment of Eligible Children by Race/Ethnicity, 20121
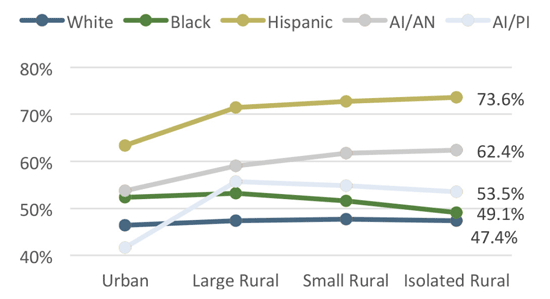
Minority children were also more likely than White children to experience a gap in health insurance coverage, particularly in rural areas. A gap in coverage is when a child has been without any type of health insurance coverage at any time in the previous 12 months.4
Impact of Coverage on Care Access
Children in rural communities are more likely than children in urban areas to experience gaps in health coverage, and enrollment in Medicaid is significantly greater in rural than urban areas, regardless of race. It is important to address care access and utilization among publicly insured populations and those with private insurance or without coverage. Studies indicate:
- Low-income rural children on public insurance were significantly less likely to have delayed seeking care compared to low-income urban children on public insurance (7.4% vs. 9.6%).6
- Parents in rural areas with private insurance for their children were more likely to report problems paying for care than were urban parents (25.3% vs. 20.5%).6
- Parents in rural areas with children on public insurance had 10% lower odds of reporting problems paying for care compared to urban parents.6
- Significantly more rural children on public insurance had difficulty obtaining referrals for care than those with private insurance (27.4% vs. 13.3%).6
Care for Rural Medicaid Children
Rural Health Clinics (RHCs) are located in rural underserved areas. Medicaid is one of their largest payers. Services at these clinics often cater to children, although there is significant variation by state.
In North Carolina, 39.1% of the RHCs' Medicaid population in 2009-2010 was children, compared to 78% of the Medicaid patient base among RHCs in Texas.7
Based on data from 2010, children have also been found to have a higher rate of emergency department (ED) use for non-emergent conditions compared to adults ages 21 and older, with the rate of ED use for non-emergent conditions generally being higher in rural areas. This may be due to lack of other options for pediatric healthcare, especially in rural areas.8
Conclusion
Poverty can make it more difficult for families with children to pay for and maintain health insurance coverage due to cost, resulting in the use public insurance. Families with children may be more likely to forgo or delay care if health insurance coverage is limited, difficult to obtain, or too expensive, resulting in poorer health for rural children. For more information on this topic, see Healthcare Access and Status Among Rural Children.
Resources
- Rural and Minority Health Research Center (2018). Characteristics of Rural Medicaid Recipients, 2012, 35 States.
- Rural and Minority Health Research Center (2016). Vulnerable Rural Counties: The Changing Rural Landscape, 2000-2010.
- Rural and Minority Health Research Center (2016). Current State of Child Health in Rural America: How Context Shapes Children's Health.
- Rural and Minority Health Research Center (2017). Trends in Rural Children's Health and Access to Care.
- RUPRI Center for Rural Health Policy Analysis (2017). Changing Rural and Urban Enrollment in State Medicaid Programs.
- Maine Rural Health Research Center (2017). The Role of Public Versus Private Health Insurance in Ensuring Health Care Access & Affordability for Low-Income Rural Children.
- North Carolina Rural Health Research and Policy Analysis Center (2016). Characteristics of Medicaid Beneficiaries Who Use Rural Health Clinics.
- North Dakota and NORC Rural Health Reform Policy Research Center (2015). Use and Performance Variations in U.S. Rural Emergency Departments: Implications for Improving Care Quality and Reducing Costs.
